Gastric Bypass Surgery: Obesity is a medical condition that occurs as a result of excessive body fat. About 36% of adults in the USA are obese. In addition, about 18.5% of children in the USA are considered obese.
By 2030 an estimated 20% of the entire world population will be obese. This is important because obesity can lead to many medical issues such as high blood pressure, diabetes, obstructive sleep apnea, cancer, and high cholesterol. These factors, unfortunately, will cause poor quality of life as well as a shorter life span.
Gastric Bypass Surgery
Bariatric surgery’s main goal is to reverse these factors to make people live a happier and longer life. Weight loss surgery has been shown most recently to increase the lifespan in patients with morbid obesity. Gastric Bypass surgery is one of these weight loss surgeries.
The surgery consists of making a small stomach pouch to limit the amount you can eat and rearranging the small intestine to cause less absorption of the food you eat, leading to fewer calories being absorbed.
The biggest question I get from patients sounds like this: Will this work for me?
What to expect one year out post-operatively.
Weight Loss With The Gastric Bypass Surgery
Statistics show that a regiment of diet and exercise alone has a 95% fail rate for long-term weight loss! So how much weight can you expect to lose with bariatric surgery? Generally, your maximum weight loss will be in the first year.
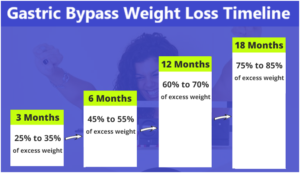
As you can see with this chart, one year after surgery, you can expect to lose up to 70% of your excess body weight. So if you’re 100 pounds overweight, you can expect to lose 70 pounds in the first year and continue to lose more weight thereafter.
Diabetes With The Gastric Bypass Surgery
The most well-known study to date and one that was done very well is the Stampede Trial. This was a randomized controlled trial where patients with diabetes were put in a medical therapy alone group or medical therapy and Gastric Bypass surgery. The end goal was a HgbA1c less than 6%.
After 1 year in the medical therapy group, 12% of the people achieved that goal. In the medical therapy and Gastric Bypass surgery group, 42% of the people achieved that goal with no medications! Another study called The Diabetes Surgery study was 19% in the medical therapy group and 49% in the gastric bypass surgery group.
Most interestingly, in the surgery group, most of them were off all diabetic medication. About 90% of people with type 2 diabetes achieve excellent results after surgery, which means they can stop their oral medications or insulin and obtain a non-diabetic HgbA1c. Most of the trials show that gastric bypass surgery is ideal for poorly controlled diabetics, especially in the severely obese.
High Blood Pressure With The Gastric Bypass Surgery
Hypertension or high blood pressure is very prevalent in obesity and is directly correlated with cardiovascular disease. In the USA, half of all patients with high blood pressure are obese.
Obesity leads to a resistance to blood pressure medication. Studies consistently have shown an improvement in hypertension in bariatric surgery patients after one year.
In gastric bypass surgery, hypertension remission rates are about 70%. In the GATEWAY (Gastric Bypass to Treat Obese Patients With Steady Hypertension), randomized trial patients on 2 or more anti-hypertensive groups were randomized to medical therapy vs. gastric bypass surgery. The primary endpoint of decreasing blood pressure medication while keeping blood pressure less than 140 was achieved in 83.7% in the surgery group and 12.8% in the medical group.
Hypertension remission, meaning coming off all blood pressure medications, happened in 50% of the gastric bypass surgery patients and none of the medical therapy patients. To summarize, after gastric bypass surgery, about 70% of patients will stop taking all their medications and have normal blood pressure. With this effect and the improvement in blood sugar and cholesterol (80% will have normal cholesterol after surgery), the risk of cardiovascular diseases such as heart attack and stroke is decreased.
GERD With The Gastric Bypass Surgery
Acid reflux disease is very predominant in obesity as the increased visceral fat leads to higher intraabdominal pressure, pushing the acid from the stomach into the esophagus leading to the typical heartburn symptoms. Gastric bypass surgery effectively relieves heartburn and is the preferred surgery in obese patients, especially as a Sleeve Gastrectomy can worsen heartburn.
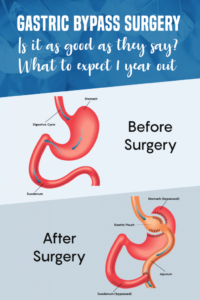
Relief of all heartburn symptoms usually happens within the first few days of surgery, and most patients will be off all their acid reflux medications. In addition, relieving acid reflux disease can help prevent long-term complications such as cancer or narrowing your esophagus, leading to difficulty eating.
Your Wellbeing With The Gastric Bypass Surgery
The New York Times reports patients who have had weight loss surgery gain long-lasting physical, emotional and social benefits compared to those who have not. In addition, weight loss surgery patients are more likely to rate themselves as healthier and are less likely to report problems with issues like pain, mobility, and depression. Physical benefits weight loss surgery provides include normalizing blood sugar and blood pressure and curing sleep apnea.
Many people with obesity are depressed with low self-esteem due to poor body image and social stigma. There is also a difficulty in doing the activities you may enjoy, which can lead to isolation and depression. Losing excess body weight can lead to the resumption of those activities and improve self-esteem. A study showed that people who underwent surgery had a 32.7% decrease in depression at the time of surgery and a 16.5% decrease in depression 12 months after surgery.
This post was originally published on ObesityHelp.com.
Dr. Pascal Bortz is a Board Certified Surgeon at Olde Del Mar Surgical and has advanced skills in laparoscopic, robotic and bariatric surgery. He earned his Bachelor of Science at the University of California San Diego and received medical school training at Saba University School of Medicine. Most recently, his project on local anesthetic to improve post-operative pain in bariatric surgery was presented at the SAGES national meeting.
You May Also Like
-
The Top Three Medical Weight Loss Solutions Explained
Feb 21, 2019
-
BMI Calculator for Bariatric Surgery
Sep 30, 2019
-
5 Summer Tips for Bariatric Exercise
Jun 19, 2019
-
3 Things to Know When Considering Weight Loss Surgery
Feb 20, 2019
-
10 Facts About Obesity You Should Know Before Surgery
Nov 05, 2019