Am I a Candidate for Weight Loss Surgery?
Get StartedTestimonials
Olde Del Mar Surgical's Patient Testimonials

My life was terrible health wise, weighed at my max 368lbs. Diagnosed with fatty liver, high cholesterol, and most importantly a diabetic. I had tried so many times to lose the weight on my own. Failed.
The best experience I have ever had with doctors. From the ladies in the office, to Rachel, the dietitian. To Kirsten and of course dr. Boyroul.
I’m more active. Able to go out and do outdoor activities with my daughter. And of course feel better health wise and look better. Has helped my self esteem as well.
Hector A.

Before I had surgery I was miserable in my own body. I felt sluggish, tired all the time, I was always out of breath, I had pain on my ankles from my weight. Sleep apnea, and acid reflux. Not being able to exercise because I was exhausted from work, coming home I would go straight to be because I had really bad ankle pain. Sometimes I would try and go for a walk, but even then I would be in pain from my ankles and just out of breath that I had barely enough energy to do anything with my son. My days off consisted of me laying in bed because I was just tired all the time.
Everyone in Del Mar Surgical have been so supportive and amazing. A HUGE thanks to Doctor Pascal Bortz and Ms. Rachel Macam, they are both really supportive and actually care for what I have to say. They are both always attentive and address any concerns that I have.
Elizabeth B

Life before weight loss surgery was always a bit challenging. It was a giant game of problem solving; what clothing do I fit in today or what can I wear to this event. I remember figuring out excuses to not go to work volunteering activities because we had to wear provided polo shirts oh, and let’s not forget the beach and pool parties that happened every weekend of my twenties. I missed out on so many things because of my weight. Avoiding situations that would make me very aware of my physical presence was my number one goal.
Del Mar surgical is wonderful. Dr. Bhoyrul and Nurse Kirsten, along with the entire staff, are so kind and warm. They have truly set me up for success, and I cannot be more thankful.
Angela W.
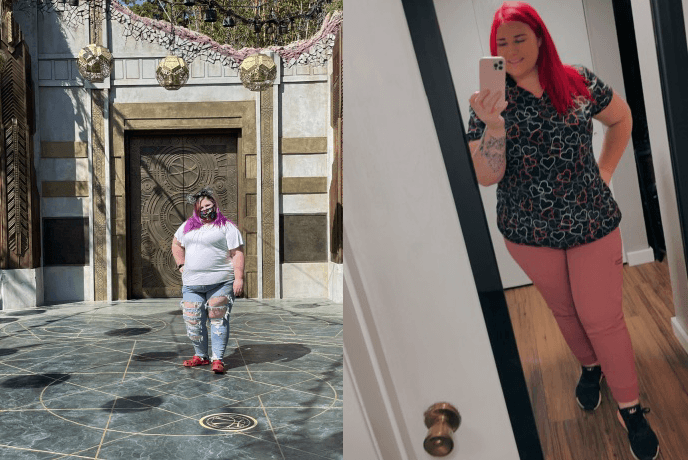
I was 350 pounds. Working in a job that I liked but never chasing my dreams of travel or flight therapy because I wasn’t comfortable in my skin. My feet always hurt, my knees started hurting and then my back. I was 27 years old and felt like a 60 year old! I had no major illnesses but pain everywhere. I couldn’t even work out because it just hurt.
Chelsea C.

My life before surgery was horrible ! Lot of physical problems, diabetes type 2 kidney infections, knee and ankle pain, problems to sleep, couldn’t walk more than a block, low sugar pressure, back pain, couldn’t play with my grandbabies couldn’t dance couldn’t ride on fair rides cause I didn’t fit ! headaches, sometimes couldn’t deeply breath. Personal life, a disaster, and depression.
Maribel I.
Are You Ready to Take Control?
Dr. Sunil Bhoyrul and the surgical team truly care about making a positive difference in the lives of our patients. Reach out today to become a success story too!